|
Mihir Bedi
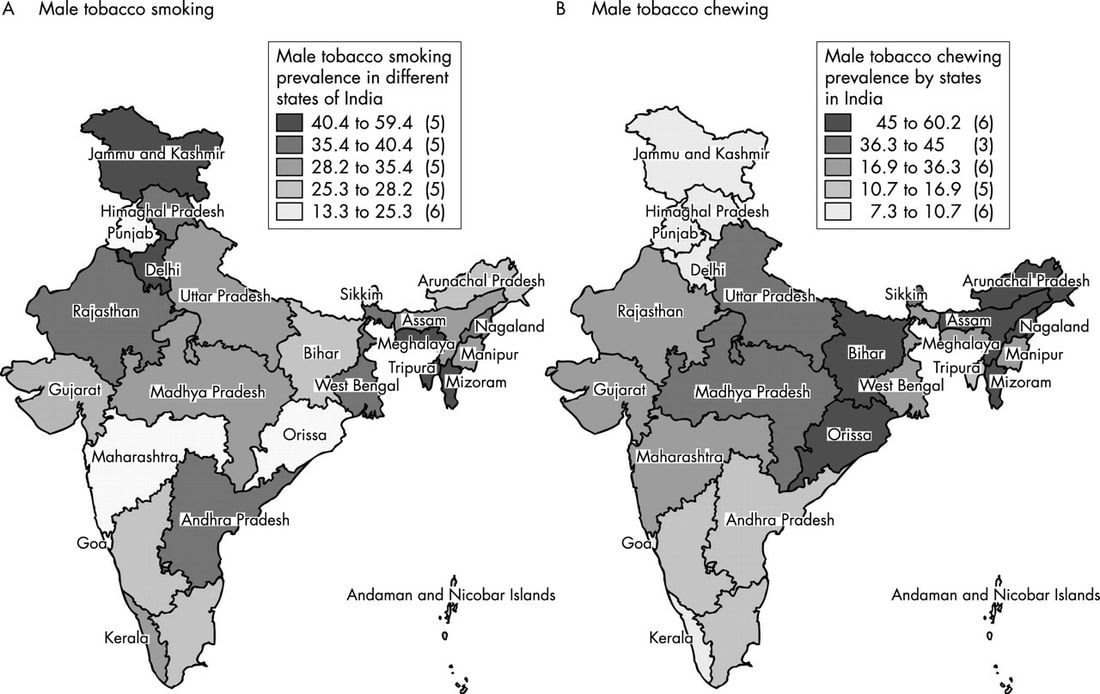
There are many biological factors that play a role in the spread of cancer, and while it is crucial to understand them, it is also important to expand our scope and consider how the spread of cancer can take place in a community of people. Even though cancer is not a communicable disease, it still has a higher prevalence in some parts of the world than others. Lung and mouth cancers, for instance, are highly prevalent in the rural regions of Rajasthan, India1. One of the most prevalent kinds of cancer in Rajasthan is mouth cancer. This prevalence of mouth cancer can be directly linked to high rates of tobacco chewing and smoking. The per capita consumption of ‘bidi,’ a cheaper form of a tobacco cigarette, is above 80,2 an alarmingly high number. Despite there being an abundance of substitutes like herbal snuff and sunflower seeds in the market, people here still consume tobacco-based products. What prompts this significant rejection of substitutes? In the rural areas of Rajasthan, India, this can be partially attributed to the low literacy rates. The entire state literacy rate is the third lowest in the nation and the rural literacy rate in 2011, as per the census survey, was merely 64%3. Even though low literacy rates resonate throughout the nation this is still an alarmingly low number when compared to the nation’s rate of 74.04%3. While working with the Samvedhna Research Foundation, I conducted a door to door survey in the village of Mangrol. According to the results of the survey, 78% of the people in the village knew that consuming tobacco causes cancer and that cancer is a life-threatening disease, yet 56% percent still chose to consume tobacco on a daily basis and consumed up to two packets of tobacco per day. The most surprising aspect of the survey was that only 8% of the people knew about the availability of substitutes. Despite regular advertisement of nicotine chewing gum and tobacco-free snuff in newspapers and on television, the survey suggested that these weren’t reaching out to the majority of people in these villages. A possible explanation for this problem can be seen by looking at the low literacy rates referenced above. These low rates might explain why individuals neglect tobacco substitutes: they do not fully understand the content of advertisements that promote their consumption. This suggests a loophole in the conventional understanding of tobacco prevention strategies in India and warrants a prevention method that goes further than simple warnings on the packets of chewing tobacco and cigarettes and advertisements. A more detailed approach would require awareness campaigns that promote the use of substitutes as well as a government-based subsidy for these substitutes. However, this is merely a short term solution to this problem. On a long term basis, the factor that plays a key role is the literacy rate. Being exposed to substitutes and understanding their purpose doesn’t completely solve the problem. Along with education comes a skill for decision making which plays a crucial role in tobacco prevention since it helps in making a rational choice between substitutes and the harmful tobacco products. When people even in rural areas are aware of the cancerous effects of tobacco products and can easily find substitutes and preventive strategies, tobacco addiction will fail to persist as a problem that plagues the entire state and nation. Sources:
0 Comments
Michelle UllmanAs wearable health-tracking technology devices are increasingly being incorporated into clothing or worn on the body as implants or accessories, the field of wearable technology itself is expanding tremendously. About 79 percent of consumers surveyed across the United States have said that technology (in the form of mobile apps, wearable devices, etc.) is important to managing their health, according to a 2019 report by Accenture (which can be found here: https://www.accenture.com/us-en/insights/health/todays-consumers-reveal-future-healthcare). Mobile apps have been quite useful in helping people track their conditions and stay healthy. For instance, Jeff Dachis, who was diagnosed with Type 1 diabetes in 2013, developed One Drop -- a company that helps diabetic patients understand and manage their condition through the use of an app. The One Drop system combines various sensors and a Bluetooth glucose meter into one app that monitors a diabetic’s blood glucose levels, food intake, exercise, and medication. It also uses an artificial intelligence algorithm to predict the diabetic’s blood glucose levels throughout the next 24 hour period, and can even suggest ways the person can control blood glucose fluctuations. It is quite user friendly, and depicts easy to understand graphics and results (as pictured below). With approximately 10 percent of the American population living with diabetes, Dachis explained that he understood that the potential market for this kind of technology was big.1 An image of the One Drop Mobile App While Dachis’ innovations are not quite in the realm of wearable technology, they set the stage for other important advances in the field that do incorporate physical devices that monitor health. For instance, some of the most recent tech-related medical treatment advances range from implants to “smart pills” that detect when patients have failed to take their medication. Spinal cord research is benefitting greatly from implant technology. This is especially notable in the case of a 29-year-old paralyzed man, who regained the ability to walk the length of an entire football field with the assistance of a walker due to an epidural electrical stimulator implant into his lower spine and six months of intensive therapy. While not a cure, this implant technology provides hope for millions of paralyzed people. Researchers at Mayo Clinic, The University of California, Los Angeles, and The University of Chicago have already started to expand their trials to bring this technology out of its experimental phase in order to make it accessible for more people. Finally, there is a new invention called the “smart pill”. Built by AdhereTech, the smart pill bottle alerts patients when it is time to take a particular medication and sends an automated text message or voicemail if they miss a dose. As many as 50 percent of people in developed countries living with chronic diseases fail to take their medications consistently as prescribed, often times out of forgetfulness (as estimated by the World Health Organization), so this kind of technology is revolutionary for combatting this.1 While it still could be modified and expanded to apply to a wider array of chronic conditions, it marks the beginning of the future of tech-based medicine. One of the current issues the industry faces is how to make this kind of health technology more affordable. Prices for these kinds of devices are currently quite high (they currently run cost $1,650 per month) and are not accessible to many Americans. Hopefully as progress is made within the field and these devices become more commonplace, more and more people will be able to take advantage of these incredible ways to track and monitor their health.
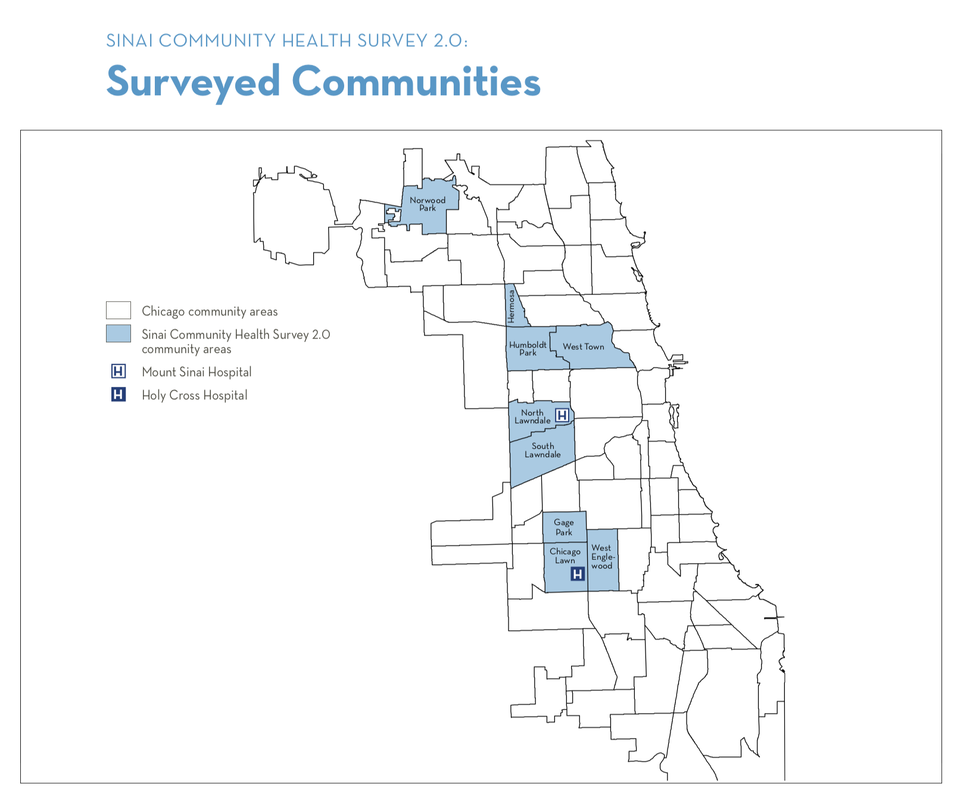
Works cited: Michelle Ullman With attention increasingly being given to affordable and accessible health care in the United States, it is necessary to focus on the underlying disparities in overall health quality and access to health care within and across various communities -- especially within the city of Chicago. Sinai Health Systems recently conducted a survey of approximately 2,000 people from nine Chicago neighborhoods to show the staggering difference in the overall quality of health across these areas (and in comparison to the health and wellness nationwide). These nine neighborhoods were Chicago Lawn, Gage Park, Hermosa, Humboldt Park, North Lawndale, Norwood Park, South Lawndale, West Englewood, and parts of West Town.1
The detailed survey (which can be found here: https://www.sinaisurvey.org) was able to make some alarming conclusions based on the data gathered. More than one in five (roughly 20 percent) of people surveyed said that they feel unhealthy. (For reference, only 12 percent of people nationally say they feel unhealthy.)2 Many people turn down medications, surgeries, and even getting prescription eyeglasses because of the unaffordable costs.3 Also, the city of Chicago’s smoking level is 18 percent, but in the selected communities surveyed, the smoking rate was found to be as high as 60 percent.2 Most of the neighborhoods are fairly even in terms of smoker gender composition, but in Hermosa, Norwood Park, Gage Park, and South Lawndale, the percentage of males who smoke is significantly higher than females who smoke.1 Health and wellness in many Chicago communities varies significantly based on factors such as race, ethnicity, income level, etc. More than half of the men surveyed in North Lawndale and West Englewood have been arrested, and many people reported experiencing domestic violence (in some communities 1/3 women reported having been a victim of domestic violence).3 Also, more than 40 percent of households in Humboldt Park, Gage Park, and South Lawndale were “food insecure” in 2016-2017 (compared to 13 percent of homes nationwide).2 These social and behavioral factors that affect health may sometimes provide more critical information than standard clinical care measures. More studies that focus on the specific social and behavioral factors that vary across communities that are (at least partially) responsible for the disparities in health quality could hopefully bring us closer to resolving some of the obstacles in our healthcare system. Works cited:
By Melanie Chow
On May 1st, the anticipated UChicago adult trauma center will finally open its doors. The $39 million facility is the city’s newest and most advanced adult emergency department, and is central to UChicago Medicine’s Urban Health Initiative (UHI). Trauma centers are usually part of an E.R, and they are there to handle extreme cases where there is an issue of immediate survival, such as traumatic car crash injuries, gun-shot wounds, stab wounds, major burns, and more. Prior to this, there were only four other trauma centers in Chicago, which were all located on the East and West side. This new center will be the only one in the South Side of Chicago, and is the product of years of community campaign and debate. By Isabelle Sohn
There are approximately 65.3 million people forcibly displaced from their homes in the world today. Within that unprecedented, gargantuan number are 21.3 million refugees, over half of whom are under the age of 18. We are now witnessing and living in an age of the highest level of human displacement ever recorded. These statistics tell us a lot about the state of the world. But often, statistics do not and cannot tell us about the experiences and difficulties swallowed up by those numbers. In particular, it can be difficult to focus on healthcare, which, while instrumental to basic human life, is not the first thing that comes to mind when considering the plights of misplaced individuals. |
Who are we?MEDLIFE strives to improve access to healthcare, education and sustainable development in underprivileged communities in Latin America, India and Tanzania. CategoriesArchives
February 2019
|


 RSS Feed
RSS Feed
